Understanding Snoring – What It Is, Why It Matters, and When to Seek Help
Dr. Arveity Setty, MD, FAASM, FAAP, DABOM
At the My TeleSleep Clinic, we often talk about one of the most common—and surprisingly misunderstood—sleep issues: snoring. While many assume snoring is simply an annoying noise and nothing more, the truth is that it can be a signal of significant sleep-health concerns. In this article we’ll cover:
- What snoring is and how it happens
- Why snoring can have clinical importance
- The main causes or “why it happens” factors
- Lifestyle and clinical interventions (how to take care of it)
- When it’s important to seek professional evaluation
Our goal is to empower you (or your loved ones) with practical knowledge—and to let you know how My TeleSleep Clinic can support you via consultations, follow-up, and home sleep study testing.
What is snoring?
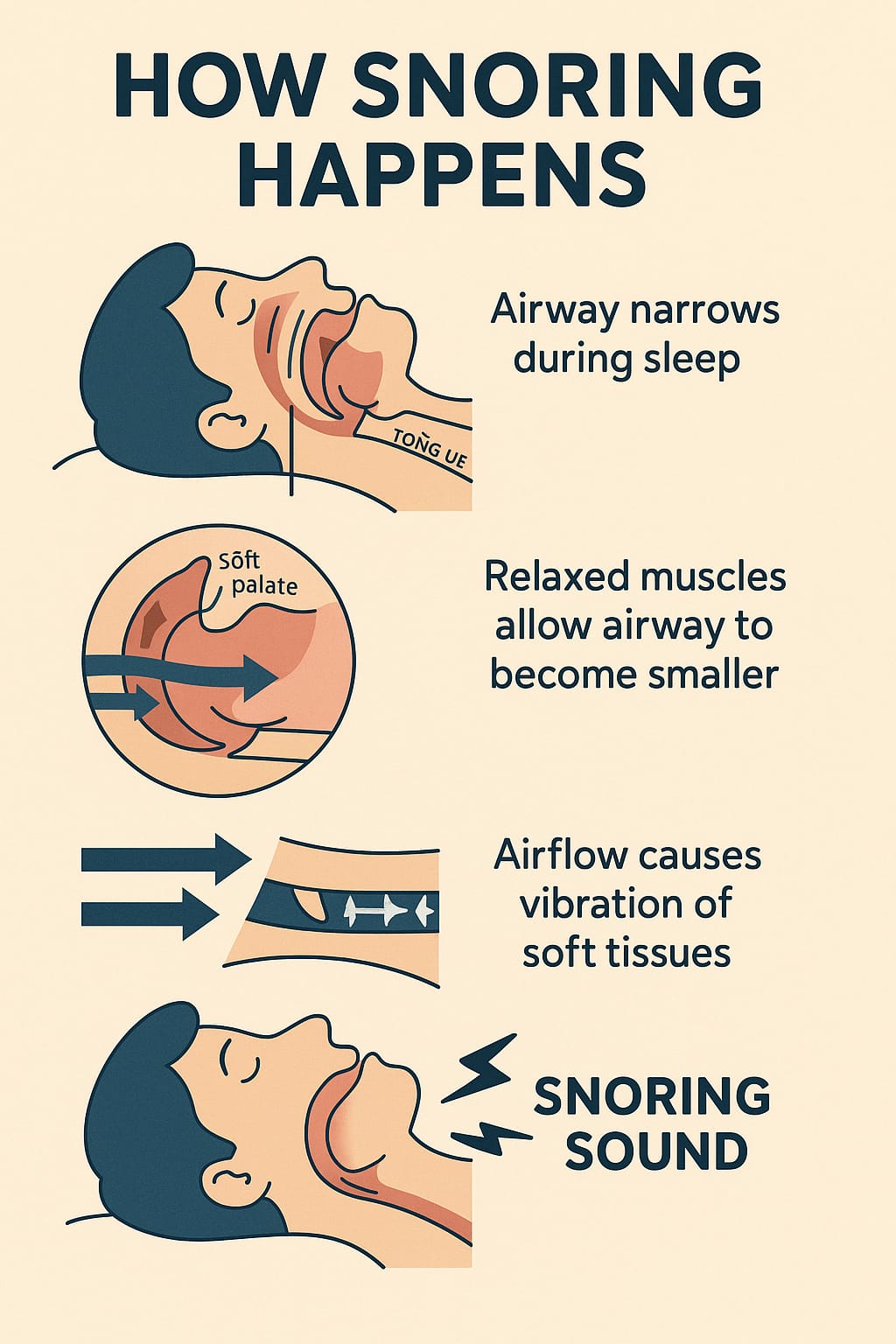
Snoring is the audible sound produced during sleep when airflow through the upper airway becomes turbulent and causes vibration of soft tissues (such as the soft palate, uvula, tongue base, or pharyngeal walls). Sleep Foundation
- The sound comes from partial obstruction of the airway (not complete cessation) causing tissue vibration.
- Not all snoring is “bad” in the sense of being a medical emergency—but it does warrant attention, especially when frequent, loud, or associated with other sleep symptoms.
- Snoring is extremely common. For example, many sources estimate a substantial portion of adults snore on some nights or regularly.
In short: snoring = a symptom (or sign) of airflow imbalance during sleep.
Why does snoring happen? (The mechanics and contributing factors)
Here are the key mechanisms and common causes behind snoring:
Mechanism – the “how”
- During sleep, muscles in the upper airway relax; this reduces tone of pharyngeal walls and the tongue base.
- If the airway is narrowed (due to anatomy, soft-tissue bulk, or external pressure), airflow becomes more turbulent; that turbulence causes vibration of tissues → sound.
- Gravity plays a role: when lying on your back (supine), the tongue and soft palate fall back more easily, increasing risk of snoring. Sleep Foundation
Contributing factors – the “why”
There are numerous risk factors or conditions that make snoring more likely:
- Anatomical factors: Deviated nasal septum, nasal valve collapse, enlarged tonsils/adenoids, long soft palate, large tongue base. UCHealth+1
- Obesity / excess weight: Extra fatty tissue around the neck/throat can narrow the airway. Sleep Foundation+1
- Age / gender: Older age and male gender tend to increase snoring prevalence (due to airway structural changes, muscle tone, fat distribution).
- Alcohol, sedative use, muscle relaxants: These further relax throat muscles so airway collapse or vibration is more likely. Sleep Foundation
- Sleep position: As mentioned, supine position favours tongue/soft palate collapse; side-sleeping may reduce snoring.
- Nasal obstruction / congestion: Allergies, colds, nasal polyps, or structural nasal problems force mouth breathing or narrow airway → snoring. UCHealth
- Pregnancy: Hormonal changes and increased tissue bulk or congestion can increase snoring risk. UCHealth
Understanding these helps both in preventing snoring and in recognising when it might be a sign of more serious issues.
The clinical importance of snoring
It is tempting to dismiss snoring as a benign nuisance—but clinically, snoring deserves respect. Here’s why:
1. Marker of possible sleep-disordered breathing
- Snoring may be a sign of Obstructive Sleep Apnea (OSA): A serious condition where the airway repeatedly partially or fully closes during sleep, leading to oxygen drops, sleep fragmentation, and cardiovascular strain. Johns Hopkins Medicine
- Even when full apnea is not present, habitual snoring can indicate upper-airway resistance, micro-arousals, and non-restorative sleep.
2. Impact on daytime functioning and quality of life
- Frequent snoring (even without OSA) may correlate with daytime sleepiness, poor concentration, fatigue, irritability.
- Partners of snorers may also suffer disrupted sleep, which has relational and health consequences.
3. Association with cardiovascular and metabolic risks
- Loud snoring (especially with pauses) has been shown to correlate with higher risks of hypertension, heart attack, stroke. AASM
- While snoring alone is not as strongly studied as OSA, the vibration and repetitive stress on the airway and cardiovascular system may contribute to vascular damage.
4. Importance of not ignoring it
- Because snoring is common and often dismissed as “just part of sleep”, many people don’t seek evaluation. But the presence of snoring combined with other symptoms should prompt a closer look.
In short: Snoring may be more than a nuisance—it may be a warning sign requiring attention.
How to take care of snoring (lifestyle + clinical)
At My TeleSleep Clinic, we emphasise a step-wise approach: start with optimising health and sleep hygiene, then escalate to clinical evaluation if needed. Here’s a breakdown.
Lifestyle and behavioural strategies
These are first-line and accessible:
- Sleep position: Try sleeping on your side instead of your back. Elevating the head of the bed slightly can also help.
- Weight management: If overweight, reducing weight can significantly improve snoring by reducing throat tissue bulk. Sleep Foundation
- Avoid alcohol and sedatives near bedtime: These relax throat muscles too much and worsen snoring. Sleep Foundation+1
- Treat nasal congestion / obstruction: Use nasal sprays for allergy, address structural problems, keep nasal passages clear.
- Good sleep hygiene: Ensure a consistent sleep schedule, avoid heavy meals right before bed, reduce smoking. Sleep Foundation
- Avoid back-sleeping: Some people use positional devices or pillows to discourage supine sleeping.
These measures may reduce snoring severity and frequency—and they are recommended whether or not a formal sleep disorder is present.
Clinical evaluation and intervention
When lifestyle measures are insufficient (or if there are red flags—more to come), clinical pathways include:
- Consultation with a sleep medicine specialist: We at My TeleSleep Clinic can assess your history, symptom burden, risk factors, and determine whether further testing is needed.
- Home sleep study (or in-lab study): If there’s suspicion of OSA or other sleep-disordered breathing, a home sleep test is often a convenient first step. At our clinic, we can arrange this for you.
- Follow-up and monitoring: If a diagnosis is made (e.g., mild/moderate OSA, or primary snoring), we monitor treatment response, adherence, and adjust plan as needed.
- Therapies: Depending on findings, options may include:
- Oral appliances (mandibular advancement devices) for snoring/OSA.
- Positive airway pressure (PAP) therapy for OSA.
- Surgical or ENT interventions if structural obstruction is identified.
- Multidisciplinary care (weight loss program, dental/sleep dentist collaboration).
- Behavioural/cognitive therapy if sleep disruption is major.
By combining lifestyle changes + targeted clinical care, many patients achieve substantial snoring improvement, better sleep, and improved health outcomes.
When should you seek a doctor? (Red flags and triggers)
It’s time to seek professional help when snoring is more than an occasional annoyance. Here are key situations to consider:
- Loud, habitual snoring occurring most nights.
- Snoring accompanied by gasping, choking, or pauses in breathing during sleep (often reported by a bed-partner).
- Excessive daytime sleepiness, morning headaches, difficulty concentrating, irritability.
- Unrefreshing sleep despite “enough” hours.
- High risk factors for OSA: obesity, large neck circumference, hypertension, cardiac disease.
- New onset snoring in pregnancy (especially with high blood pressure/preeclampsia risk).
- Worsening snoring despite lifestyle changes.
- Snoring plus other ENT issues (nasal obstruction, enlarged tonsils, recurrent sinusitis).
- Partner or sleep environment significantly impacted by the snoring (bed‐sharing disrupted, sleep deprivation).
In all of these cases, it’s wise to reach out. At My TeleSleep Clinic we offer a comprehensive sleep medicine consultation, assess your risk, and if indicated, arrange a home sleep study. Early detection and management can prevent more serious downstream effects (cardiovascular, metabolic, cognitive) associated with untreated sleep disorders.
Why choose My TeleSleep Clinic?
- We specialise in sleep medicine and have experience with snoring and sleep-disordered breathing.
- Virtual consultations make it easy—especially if you have busy schedule or live in a remote area.
- We coordinate home sleep studies, allowing you to test in your own bed, making the process more comfortable and convenient.
- We provide follow-up care, monitoring your progress, making adjustments, and ensuring that treatment is working for you.
- Our approach is holistic: We address lifestyle, anatomy/physiology, and underlying medical factors—not just “snore reduction”.
In summary
Snoring is more than just a noisy nuisance—it can be the tip of the iceberg for sleep-related breathing issues. Understanding the “what”, “how”, and “why” empowers you to take action. With the right combination of lifestyle habits and clinical oversight, many people reduce snoring, sleep better, and improve overall health.
If you find yourself or a loved one snoring regularly, especially if accompanied by other symptoms (daytime fatigue, gasps, observed pauses), we encourage you to schedule a consultation with us at My TeleSleep Clinic. Let’s find out what’s going on—and help you get the restorative sleep you deserve.
Take the Next Step Toward Quiet Sleep
Snoring isn’t a life sentence for you or your partner. It is a treatable mechanical issue.
If you suspect your snoring is affecting your health or your relationship, don’t guess. Get tested. At TeleSleep Clinic, we offer convenient home sleep testing and virtual consultations with sleep specialists who can guide you toward the right, evidence-based solution.
Stop merely surviving your nights and start resting.